Types of Neuroacanthocytosis
Exploring Neuroacanthocytosis might seem puzzling. Knowing its different types is key to simplifying this uncommon nerve disorder. By exploring the various categories, one can gain a deeper comprehension of the intended meaning by all parties involved.
1. Chorea-Acanthocytosis (ChAc):
Overview:
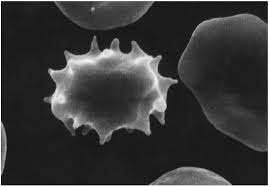
ChAc is one of the main types of Neuroacanthocytosis. It leads to a specific movement disorder called chorea. Chorea causes the kind of movements once described as flapper ladies. The arms and legs jerk and move very suddenly, like someone doing a dance against their will.The term “acanthocytosis” refers to the funny shaped red blood cells that build up in the blood in this type of Neuroacanthocytosis. It is an important feature of Neuroacanthocytocis.
Symptoms:
- Involuntary Movements: Jerky and unpredictable dance-like movements.
- Muscle Weakness: Weakening of muscles, impacting coordination.
- Cognitive Changes: Disturbances in cognitive functions.
2. McLeod Syndrome:
Overview:
McLeod Syndrome presents another face of Neuroacanthocytosis. In this type, the focus extends beyond the abnormal shapes of red blood cells to include various neuromuscular and psychiatric symptoms. McLeod Syndrome is characterized by a deficiency of certain blood proteins, particularly XK, leading to a broader spectrum of clinical manifestations.
Symptoms:
- Muscle Trouble: Weak, disappearing muscles.
- Thinking Changes: Memory and mind tasks shift.
- Mood Problems: Feelings and actions alter.
3. Huntington’s Disease-like 2 (HDL2):
Overview:
There’s a brain disorder called HDL2. People also know it as Huntington’s Disease-like 2. This particular disorder falls within the category known as Neuroacanthocytosis. it shares similarities with Huntington’s Disease in various aspects. However, unlike ChAc or McLeod Syndrome, HDL2 may not manifest symptoms as swiftly. Nonetheless, over time, HDL2 gradually weakens the brain, affecting both motor skills and cognitive abilities.
Symptoms:
- Movement Disorders: Involuntary movements and chorea.
- Cognitive Changes: Progressive decline in cognitive functions.
- Behavioral Disturbances: Changes in mood and behavior.
4. Neuroferritinopathy:
Overview:
Neuroferritinopathy adds a new layer to the complexity of Neuroacanthocytosis. This particular form is characterized by the abnormal accumulation of iron in specific regions of the brain, which gives rise to a range of neurological symptoms. Neuroferritinopathy, although not as common as some other types, highlights the diverse nature of the Neuroacanthocytosis spectrum. It serves as a testament to the wide range encompassed within this condition.
Symptoms:
- Movement Disorders: Involuntary movements, akin to chorea.
- Cognitive Impairment: Changes in memory and cognitive functions.
- Psychiatric Features: Mood disturbances and personality changes.
5. PLA2G6-associated Neurodegeneration (PLAN):
Overview:
Neuroacanthocytosis Genetic Variant Known as PLAN (PLA2G6-Associated Neurodegeneration) This change in the PLA2G6 gene leads to various brain disorders. PLAN is a broad term. It covers many types of clinical signs, showing how genes affect different types of brain conditions.
Symptoms:
- Movement Disorders: Uncontrolled Motions and Stiffness in Muscles
- Cognitive Decline: A Progressive Breakdown
- Neurological Regression: Decline in Proficiency and Capabilities
Global Prevalence of Neuroacanthocytosis:
Obtaining precise global prevalence data for Neuroacanthocytosis poses a challenge due to limited research and varying diagnostic practices. However, some studies suggest:
- Europe: Chorea-acanthocytosis prevalence ranging from 1 in 50,000 to 1 in 200,000.
- Japan: McLeod syndrome estimated to affect about 1 in 100,000 males.
- North America: Limited data, but estimates suggest similar prevalence to Europe for Chorea-acanthocytosis.
These figures again emphasize the rarity of Neuroacanthocytosis across different regions. Nonetheless, as further research progresses and diagnostic capabilities improve, there is a possibility of uncovering a more comprehensive understanding of its global prevalence in the future.
Complications of Neuroacanthocytosis
Complications of Neuroacanthocytosis are quite extensive and can vary depending on the specific type:
General complications:
- Progressive neurological decline: This can manifest as worsening movement disorders, cognitive decline, and impaired speech.
- Psychiatric disturbances: Depression, anxiety, and even psychosis can occur in some individuals.
- Pain and fatigue: Chronic pain and debilitating fatigue are common symptoms that can significantly impact quality of life.
- Nutritional deficiencies: Issues with swallowing or absorbing nutrients can lead to deficiencies and further health complications.
- Respiratory problems: Respiratory weakness and infections can pose additional challenges.
- Cardiac complications: Some types, like McLeod syndrome, can increase the risk of heart problems.
- Gastrointestinal issues: Constipation, diarrhea, and other digestive issues can be recurrent.
- Seizures: Epilepsy is a potential complication in some types of Neuroacanthocytosis.
- Death: Sadly, premature death can occur in some cases, particularly with severe or rapidly progressing forms.
Specific complications by type:
- Chorea-acanthocytosis: Anemia due to acanthocytes, liver and kidney dysfunction, and intellectual disability.
- McLeod syndrome: Cardiac arrhythmias, heart failure, and increased risk of infections.
- Huntington’s disease-like 2: Pronounced gait and balance problems, swallowing difficulties, and vision impairments.
- Pantothenate kinase-associated neurodegeneration: Sleep disturbances, hormonal imbalances, and severe muscle rigidity.
Neuroacanthocytosis life expectancy
Affected individuals usually live for 10-20 years after symptom onset. However, this can vary significantly depending on the specific type of Neuroacanthocytosis, individual case variations, and timely access to proper management. Some individuals, particularly with milder forms and effective symptom management, may enjoy longer lifespans.
What is the inheritance pattern of Neuroacanthocytosis?
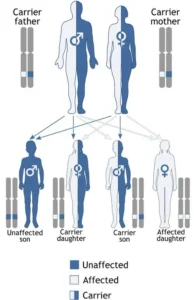
The inheritance pattern of Neuroacanthocytosis depends on the specific type, as each involves mutations in different genes and follows distinct genetic rules. Following are the inheritance pattern of given types
1. Chorea-acanthocytosis (ChAc):
- ChAc follows an autosomal recessive inheritance pattern.
- The fact is, each parent should have one VPS13A mutant gene for their child to be impacted.
- People with just one mutant gene (known as carriers) usually don’t show signs.
- In each scenario when the mum and dad both have it, the odds for the baby to get it in each pregnancy are 25%.
2. McLeod Syndrome:
- McLeod Syndrome follows an X-linked recessive inheritance pattern.
- This means that the mutated XK gene is located on the X chromosome, and males are much more likely to be affected than females.
- Males with one copy of the mutated gene will have McLeod Syndrome, while females with one copy will usually be carriers and may have mild symptoms in rare cases.
- Daughters of an affected male have a 50% chance of being carriers, while sons have a 50% chance of being unaffected.
3. Huntington’s disease-like 2 (HDL2):
- HDL2 also follows an autosomal recessive inheritance pattern, similar to ChAc.
- A kid gets ill when both mom and dad hold a flawed JUNPH gene each.
4. Pantothenate kinase-associated neurodegeneration (PKAN):
- PKAN also follows an autosomal recessive inheritance pattern, similar to ChAc and HDL2.
- For a child to be affected, it is necessary for both parents to carry a singular copy of the mutated PANK2 gene.
- In each pregnancy, when both parents are carriers, there is a 25% chance of their child being affected.
